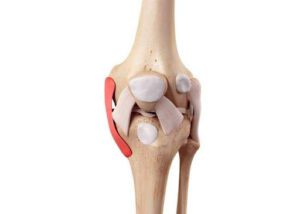

The MCL is one of the most commonly injured ligaments in the knee. Injuries to the MCL can range from mild sprains to complete tears, and can be caused by a variety of mechanisms.
Mechanism of MCL injury include:
- A direct blow to the outside of the knee causing a valgus stress and force to the inside of the knee,
- A twisting or bending of the knee, causing a valgus stress and force through the MCL
- Or, a sudden change of direction while running or jumping.


MCL injuries are classified based on the severity of the injury:


- Grade 1: A grade 1 MCL injury is a mild sprain where the ligament is stretched but not torn. Common symptoms of grade 1 include:
- Mild pain, swelling, and tenderness on the inside of the knee.
- Some slight sensation instability.
- You will most likely tolerate walking and find a deep squat or walking up/down stairs difficult.
- Grade 2: A grade 2 MCL injury is a partial tear of the ligament. Symptoms may include:
- Moderate pain, swelling, tenderness,
- Bruising on the inside of the knee,
- Knee feels unstable,
- May be some difficulty putting weight on the affected leg
- Grade 3: A grade 3 MCL injury is a complete tear of the ligament. Symptoms may include:
- Severe pain, swelling, tenderness,
- Severe bruising on the inside of the knee,
- Very unstable feeling of knee,
- Significant difficulty bearing weight on the affected leg.
In addition to the MCL, other structures in the knee joint can also be damaged in an MCL injury. These include, the medial meniscus (a C-shaped cartilage structure that cushions the knee joint) or the anterior cruciate ligament (ACL). Damage to these structures can increase the severity of the injury and may require additional treatment.
Treatment:
Regardless of the severity of the MCL injury, it will often be treated nonoperatively with promising outcomes. Surgery may be indicated when the MCL occurs concomitant with an avulsion fracture or injury to surrounding structures, as well as if knee instability remains following conservative management.
Swelling and pain management:
- Ice:
- Apply ice to the knee to help reduce pain levels
- General application includes 15-20 minutes every 2-3 hours during the initial 48 hours.
- Compression:
- Use a compression bandage or tubi-grip to help control swelling.
- Ensure that the compression is snug but not too tight, as excessive compression can cause additional circulation issues.
- Elevation
- Elevate the leg, when possible, to further reduce swelling.
- Keeping the knee elevated above the level of the heart is a useful way to judge how high to elevate.
- Medication
- Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, may help alleviate pain and reduce inflammation.
- However, it’s important to consult with your doctor before using these medications.
Modified weight bearing: Depending on the injury classification (grade 1+), you may benefit from using crutches to off-load the knee and assist with pain management, while minimising the stretch on the MCL.
Brace: A knee brace can be helpful if the knee is feeling unstable. Depending on the severity of the sprain, your physiotherapist may initially lock the brace into a reduced range to prevent the knee from straightening and bending all the way. Braces are a great way to reduce pain and instability, improve function and prevent further MCL injury
Physiotherapy: Used to help assess the injury classification and initial individualised treatment. Following and in most cases during the initial phases of treatment, physiotherapy will help you restore movement and strength, leading to an efficient return from injury. If you are wearing a brace, it should be removed several times a day to carryout exercises to ensure movement remains in the knee joint.
As initial treatment commences, progressive strategies used by your physiotherapist include:
- Range of motion exercises:
- Individualised exercises to improve and maintain the range of motion of the knee joint
- Gentle, controlled movements help prevent stiffness and promote healing. These are steadily progressed throughout your treatment and assist in guiding you back to full recovery.
- Strengthening exercises:
- Specific strengthening exercises target the muscles around the knee, including the quadriceps, hamstrings, calf muscles and the gluteal complex.
- Strengthening these muscles provides additional support to the knee joint and is paramount to your recovery.
- Proprioception Training:
- Proprioception refers to the body’s ability to sense its position in space. MCL injuries can affect this sense of joint position.
- You physiotherapist will incorporate exercises that challenge balance and proprioception to enhance joint stability.
- Functional training:
- As the MCL heals and your range of motion and strength returns, functional training becomes vital. This includes exercises that mimic daily activities or specific movements related to sports or work.
- Functional training helps ensure that the knee is prepared for the demands of real-world activities.
- Manual Therapy:
- Your physiotherapist may use hands-on techniques, such as joint mobilisation or massage, to improve tissue mobility and reduce the sensitivity of the knee and surrounding muscle groups.
- Manual therapy can complement exercise and help optimise recovery.
- Progressive Rehabilitation (Overload):
- Your physiotherapy program is often structured in a progressive manner, gradually increasing the intensity and complexity of exercises as your MCL injury improves.
- This progression is tailored to your specific needs and goals.
- Education and Home Exercises:
- Education and understanding of your condition, accurate movement patterns, and strategies to prevent reinjury (as much as possible), is an important and necessary strategy used throughout your treatment journey.
- Home exercise programs are often provided to reinforce the gains made during in-clinic sessions.
- Return-to-Activity Guidance:
- Based on your range of motion, strength, plyometric training, proprioception and further testing, your physiotherapist will determine the appropriate time to return to sports or other activities.
For an MCL, symptoms often take 6-8 weeks to settle and it can take 3-4 months to fully recover from a grade 3 MCL tear. Recovery will be more efficient if you keep up with your exercises and guidance provided by your physiotherapist. A combination of strengthening and movement exercises should be completed daily.
The specific exercises for an MCL injury depend on the severity of the injury and the stage of the healing process. It is important to work with your physiotherapist to develop a personalised exercise program that is safe and effective for your specific needs and goals.
A Guide to MCL Rehabilitation
Phase 1:
In the acute phase, within the first few days of the injury, protection of the injured tissues is recommended with rest, ice, elevation, brace and gentle range of motion exercises. The aim of this phase is to control swelling and pain, regain quadriceps function and activation, restore flexion and extension range, and normalise gait patterns.
Phase 2:
In the mid-stage of MCL injury rehabilitation, strength, dynamic balance and plyometrics are the focus. The exercises within this phase will aim to increase knee stability and prepare the knee for returning to running by the end of phase 2.
Strength component consists of quadricep, hamstring and calf exercises.
Squats: progressing with weights and/or single leg when able. Examples of strength exercises can include:
- Reverse step ups
- Resisted knee extension (within suggested range of motion)
- Romanian Deadlifts
- Hamstring curls
- Standing calf raises: progressing to single leg and range off a step
- Seated calf raises: progressing with weights (ie. Dumbbell or kettle bell on knee).
Balance: Ligaments play an important role in proprioception and balance and therefore need to be retrained following an injury. Balance training for an MCL includes:
- Y-balance
- Superman
- SL stance with eyes closed
Plyometrics: Prior to beginning plyometric training, it is generally recommended that the following is achieved:
- Full knee extension range of motion
- At least 120° of knee flexion
- Ability to demonstrate a stable, pain free bilateral squat
- Quadriceps strength of at least 70% compared to the uninjured side.
When these have been achieved, plyometric exercises should start with straight line and progress to lateral movements that challenge the MCL, which can look like:
- Box Jumps
- Single leg hops
- Lateral shuffle
- Lateral box jump
Phase 3: Returning to Sport
The late-stage of MCL injury rehabilitation, it is intended to increase the volume, intensity, and complexity of your training. This is done in order to adequately prepare you for return to sport and competition.
The criteria to return to sport is that the injured leg has strength, power and stability of at least 95% of the uninjured leg.
This phase will also consist of drills including:
Straight line running, working up intensity to sprinting. A return to running program will be provided by your physiotherapist.
Multidirectional drills, cutting and lateral movements.


The following return-to-sport continuum is used to create a visual guide when returning to sport.
Return to Participation: beginning to participate sports specific drills and modified training.
Return to sport: participating in full training. This may take several months to get to pre-injury levels
Return to performance: playing competitively when at pre-injury or greater level.
If you have experienced a recent knee injury, or, you have persistent knee pain, please do not hesitate to contact our friendly and experienced team at Any Stage Physiotherapy and Sports Medicine. We are here to guide you back to a pain free lifestyle and help return you to physical goals.
Authors


Daniel Lee
DPT, B. Sc, APAM
Director / Principal Physiotherapist
Daniel Lee has created a specialised approach to Physiotherapy treatment, return to sport and injury prevention by incorporating a functional strength & conditioning approach, no matter the individual’s age, sport, lifestyle, or competition level.

Shannon Murray
DPT, B. HSc, APAM
Physiotherapist
Shannon completed her Doctor of Physiotherapy degree at Macquarie University, after relocating from Queensland, where she completed her Bachelor of Health Science degree. Whilst completing her Doctor of Physiotherapy degree, she gained valuable experience in various setting, including private practice and hospital.









